In November 2022 I laid out my thoughts on the mechanisms underlying causes and opportunities for recovery from Long COVID (LC). That post, Mitochondria Get Center Stage, explained many of the basics of why and how mitochondria are relevant to the LC and how I applied this understanding to my own recovery.
In recent weeks the scientific literature is filling up with new articles about the role of mitochondria in COVID and especially LC. One important abstract is on the website of 08-16-23 edition of Science Transitional Medicine, “Core mitochondrial genes are down-regulated during SARS-CoV-2 infection of rodent and human hosts”.
The editor’s comments lay out a key finding “the virus is able to block expression of both nuclear-encoded and mitochondrial-encoded mitochondrial genes, resulting in impaired host mitochondrial function.” This information is highly relevant to current research and to the development of successful treatments for Long COVID.
During the height of the pandemic, many, if not most scientific and medical journals made COVID research freely available. I mention this because, despite the relevance of the article from Science Translational Medicine, it is behind a pay wall. The pandemic is not over. Cases are again on the rise and millions of individuals worldwide are struggling with the consequences of Long COVID. This, and other current research, need to be published ‘open access’, freely available to professionals and the public.
Based on the increased interest in mitochondrial dysfunction in Long COVID, parts of my previous post are included below.
(From 11-28-22) It’s tempting to consider laying out the protocol that’s been useful and effective for me, but I believe that it would be a disservice. Successfully addressing Long COVID will require understanding and addressing the causes. Treating symptoms appears unlikely to cure Long COVID.
My hope is that individuals and professionals can use this information and perspective to tailor treatments that address the causes. Policy makers need to pay attention. Decisions made by various institutions can either support resolution or extend personal and societal suffering that have been brought on by Long COVID.
I’m honored that to date, readers include a wide range of individuals. Thank you for understanding that some of what you read here might include lessons from a biology class that you took years ago and have long since forgotten.
If you’re an expert and some of what you read here lacks the nuances that are common in journal type publications, thanks to you too for understanding the need for simplicity. Please use the comments section if you want more information or want to share your insights. Also, please feel free to challenge my assumptions.
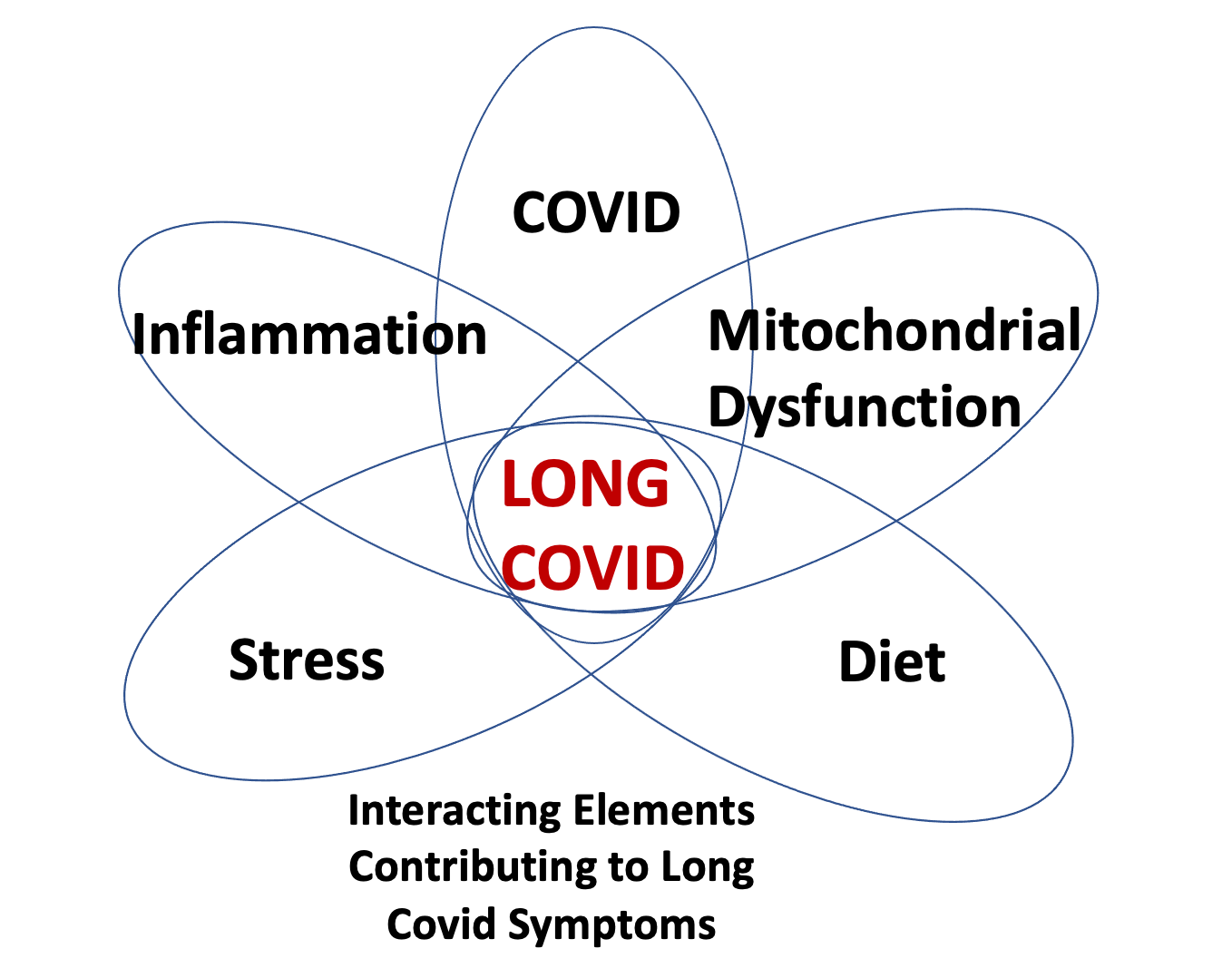
The Long COVID diagram above shows five interacting elements. All of them are important. All were involved in my illness, and all have been involved in my recovery.
An example is diet. I’ve had to pay attention to diet after discovering that I’d developed new food sensitivities during my early encounter with COVID-19. Certain nourishing foods that I’d once enjoyed had become highly inflammatory to my system. This early insight gave me hope and opened the small window that I mention in the introductory post.
I will get back to each of these five elements individually as well as to discuss the evidence of how they appear to be interacting in Long COVID. But in this post, mitochondria are going to get center stage.
Mitochondria are tiny organelles that are found inside cells. Millions of these vital mitochondria play important roles in our bodies. They are best known for production of energy to fuel all body functions. That means that mitochondria provide necessary energy for our nervous system including the brain, other organs such as heart, lungs, digestive tract, our muscles and much more.
Less often discussed are the roles of mitochondria in immune responses. As part of the innate immune system, mitochondria recognize the presence of invading viruses and help to clear the body of viral infections.
Evidence suggests that Long COVID is, in part, the result of COVID-induced mitochondrial dysfunction (1-3) made chronic (ongoing) by one or more sources of inflammation, dietary issues and stress.
Mitochondria are a source of inflammation and, at the same time, vulnerable to damage from stress and inflammation. Here, stress means both environmental and cellular stresses that are part of normal biological and disease processes.
Fortunately, these tiny warrior-energy producing factories have the capacity to self-repair. That process is called biogenesis.
In this process mitochondria can discard damaged sections (fission) and merge (fusion) with other mitochondria. Increased numbers of mitochondria can also be produced by this process. In this way, mitochondria can meet the changing needs of the body.
When the Sars-CoV-2 virus (the virus that causes COVID) enters a cell, it locates itself on the membrane walls of mitochondria and other internal cell parts. Scientists have shown that the virus disrupts normal processes and uses the cell’s energy to support viral replication. This deprives the human host of normal energy supply. Fatigue, brain fog and muscle weakness are easily understood in the context of a body competing with the virus for necessary energy.
Cell processes and the battles with the virus result in inflammation. In short, the millions of warrior-energy factories are damaged. This results in mitochondria that cannot work normally, what is called mitochondrial dysfunction.
The good news is that mitochondrial dysfunction is not new. Physicians and scientist have devised solutions for treating it. One comprehensive example comes from a group that proposed care for post-ICU patients who were experiencing mitochondrial dysfunction (4). In their model and elsewhere, treatment involves readily available nutritional support (food and over the counter supplements).
This was, for me, the place to start to recover. Later, when my energy level began to normalize, I added other strategies that favored restoring mitochondria to the pre-infection levels of vitality.
Resolution of Long COVID for me also involved reducing sources of inflammation throughout my body. Antihistamines and anti-inflammatories were not effective in addressing the inflammation. In my case it was apparently associated with gastrointestinal (GI Tract) inflammation. For me, it unequivocally required a change in my diet.
Fortunately, my sense of humor and my training in mucosal immunology and endocrinology were still in tack. More on diet in my next post.
A note on these references. They represent just a few of many high-quality peer reviewed journal articles addressing viral-mitochondrial interactions. Links to other peer reviewed quality articles are welcome in the comments section.
(1) KK Singh, et al., Decoding SARS-CoV-2 hijacking of host mitochondria in COVID-19 pathogenesis, 20 JUL 2020 https://doi.org/10.1152/ajpcell.00224.2020
(2) S Ajaz, et al., Virus-Host Cell Interactions and the Viral Life Cycle: Basic Science to Therapeutics: Mitochondrial metabolic manipulation by SARS-CoV-2 in peripheral blood mononuclear cells of patients with COVID-19- American Journal of Physiology-Cell Physiology, 2021
(3) Costa TJ, et al., Mitochondrial DNA and TLR9 activation contribute to SARS-CoV-2-induced endothelial cell damage. Vascul Pharmacol. 2022 Feb;142:106946. doi: 10.1016/j.vph.2021.106946. Epub 2021 Nov 25.
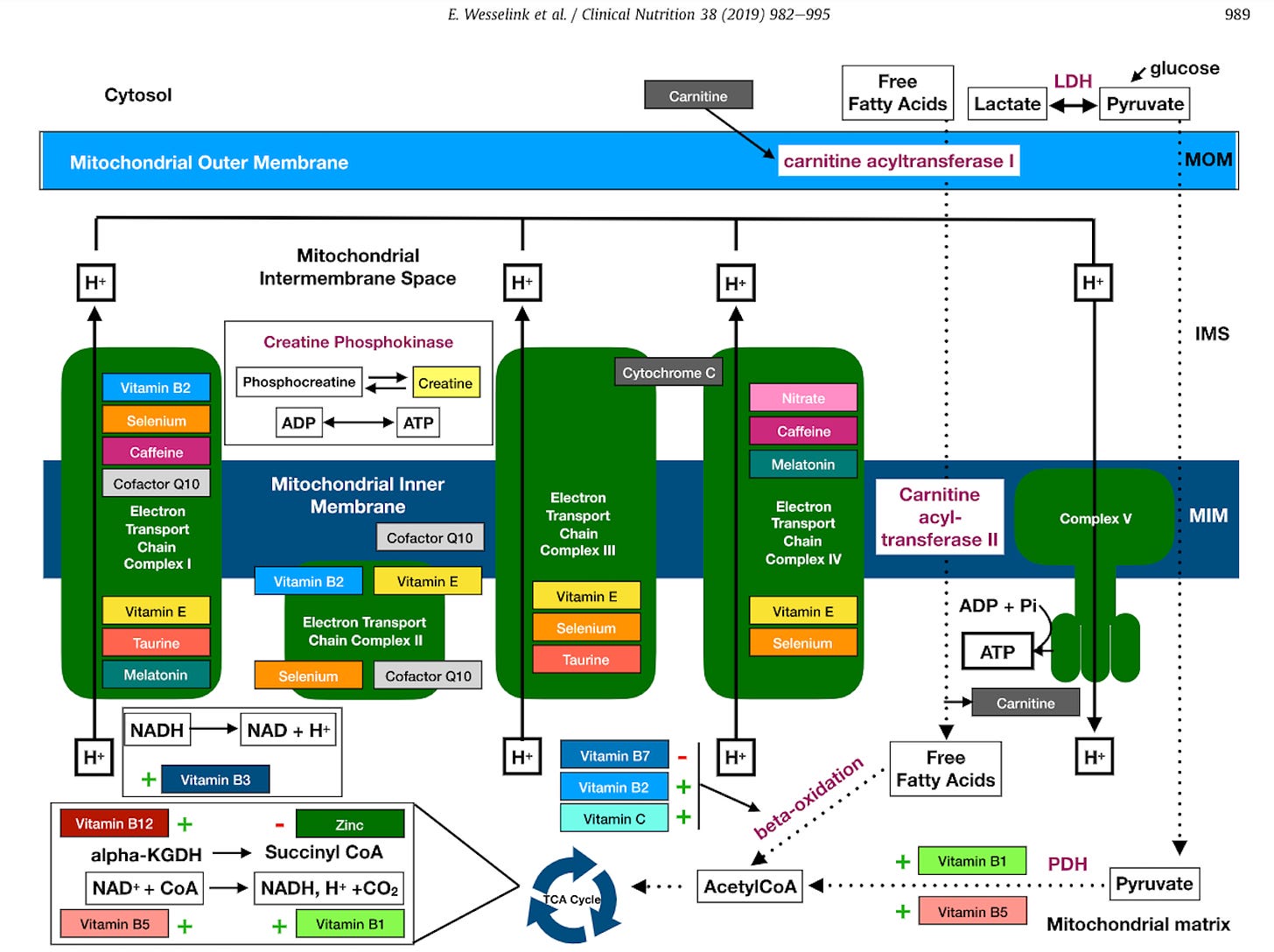
(4) Wesselink, E, et al.,Feeding mitochondria: Potential role of nutritional components to improve critical illness convalescence. Clinical Nutrition, 2018, https://doi.org/10.1016/j.clnu.2018.08.0320261-5614/© 2018 The Authors. Published by Elsevier Ltd. This is an open access article under the CC BY-NC-ND license (http://creativecommons.org/licenses/by-nc-nd/4.0/).
Vermont is still recovering from the recent floods. While free subscriptions are available, I will donate 50% of all new paid subscriptions through the end of September 2023 to VT Flood Response & Recovery Fund at the Vermont Community Foundation.


Hello! I’m grateful for your informative post and feel rather desperate to understand how to assist my own mitochondria in repair... without the ability to fully follow all the science. Is there a “mitochondrial support for artists” platform somewhere? I’m using what tiny residual executive function I have to keep working and avoid total financial collapse… Then my weary mind tries to find hope in the long Covid community, but I’m frustrated by the lack of energy to research and learn the relevant science! Would so love a shorthand to mitochondrial support for the average Jane.
I was of this mind as well but doctors where I live are very...well... unconcerned. Ketogenic diet was like hitting a home run. My mitochondria were super performing, life was great, then covid (4/2020). Mild case left with no energy. I couldn't figure it out but I wasn't producing any keytones and my blood sugar was staying around 110. I broke my fat metabolism somehow. Gluconeogenisis was trying to keep me alive? Anemia, neurological problems, etc. Couldn't get a doctor interested to save my life literally. Long story short but supplementing with some key vitomers. seems to be helping a lot (methyl folate) I wish mainstream doctors would become interested but I suppose this is why you write! Thank you.
Richard W Roberts